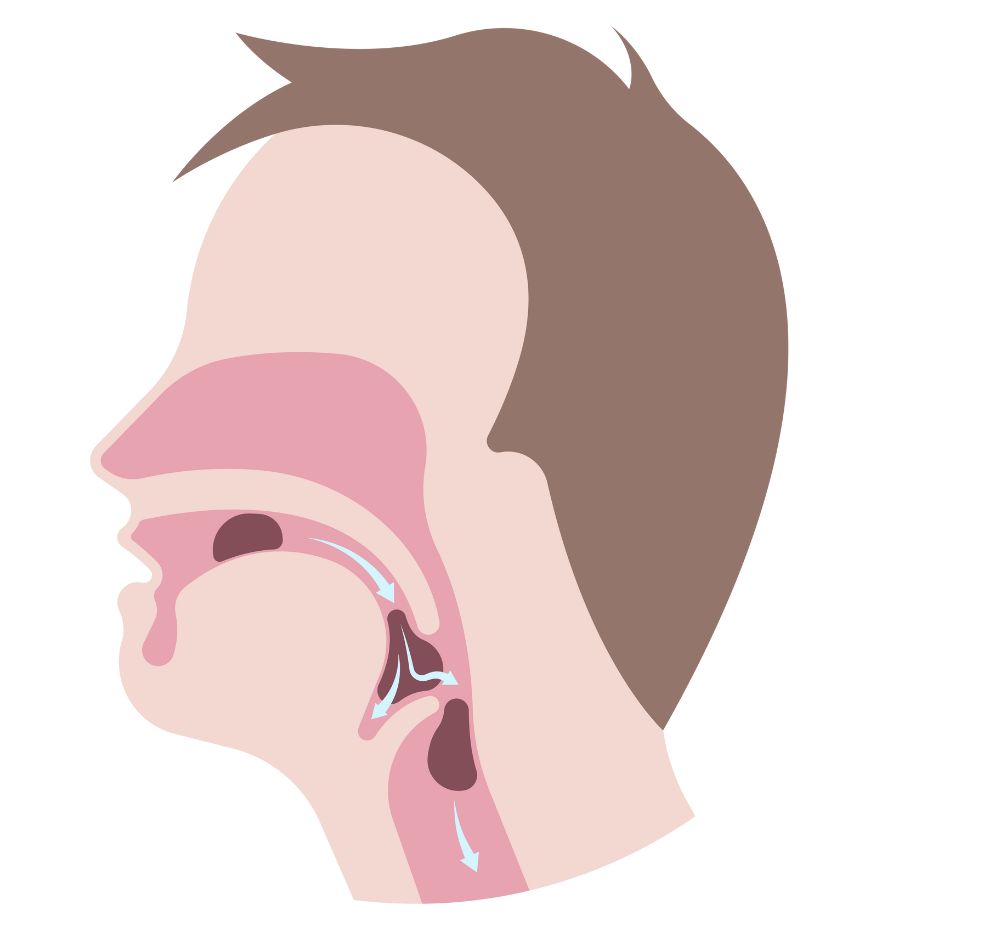
Dark Circles, Silent Clues: Could a Breathing Disorder Be the Culprit?
Venous pooling, refers to the dark discoloration that appears under the eyes. This condition is often caused by an underlying issue with the blood vessels and can be exacerbated by problems with breathing or the airway.
It is commonly known that if a person has dark circles under their eyes they are most likely tired. Could there be more to it? We are going to explore the link between bags/dark circles under the eyes and the connection to airway issues and allergies.
Venous pooling, or periorbital dark circles, refers to the dark discoloration that appears under the eyes. This condition is often caused by an underlying issue with the blood vessels and can be exacerbated by problems with breathing or the airway.
Here is how airway issues can lead to venous pooling under the eyes. Venous pooling happens when blood collects or stagnates in the veins, causing the area under the eyes to appear dark or bluish. This is due to the thin skin under the eyes, which makes the underlying blood vessels more visible. Proper blood flow is essential for delivering oxygen and nutrients to tissues and removing waste products. When blood flow is restricted or slowed down, it can accumulate in certain areas, leading to discoloration.
Airway issues, particularly those affecting breathing during sleep, can significantly impact venous blood flow.
Chronic nasal congestion or obstructions force individuals to breathe through their mouth. This can alter the normal airflow dynamics and increase the pressure in the veins around the nose and eye, leading to pooling. Obstructive sleep apnea (OSA) is a condition where the airway is repeatedly blocked during sleep, causing brief cessations (stops) of breathing. These episodes cause fluctuations in blood oxygen levels and pressure, affecting blood vessels, including those under the eyes. Chronic sinusitis or allergies can lead to swelling of the nasal passages, increasing venous pressure in the facial area. This can result in the appearance of dark circles due to venous pooling.
Airway obstructions can lead to increased intrathoracic pressure during breathing, especially when the individual struggles to inhale air. This pressure is transmitted to the facial veins, leading to engorgement and pooling.
Airway issues can also affect the lymphatic system, which is responsible for draining excess fluid buildup and venous pooling under the eyes.
Episodes of hypoxia (low oxygen levels) due to airway obstructions can cause the blood vessels to dilate to increase blood flow and oxygen delivery. This vasodilation can make the blood vessels under the eyes more prominent.
So how can we prevent this?
Addressing nasal obstructions, allergies or sinus issues.
By involving a myofunctional therapist in your treatment plan to help with nasal breathing and tongue posture that will then aid in sleep and breathing.
Incorporating a nasal hygiene routine in your day to help manage symptoms.
Addressing the root cause of airway issues can lead to improved overall health and a reduction in the appearance of dark circles under the eyes.
Correcting the Hidden Habit: The Key to a Proper Swallow & Myofunctional Therapy
Correcting the Hidden Habit: The Key to a Proper Swallow in Myofunctional Therapy.
Swallowing is a fundamental habit that most of us take for granted. However, improper swallow patterns, often called “tongue thrust” can lead to a variety of dental and health issues. In myofunctional therapy, addressing these issues is key to achieving better overall health. In this week’s blog we will explore the importance of proper swallow techniques and the issues that an improper swallow technique can create. As well as how myofunctional therapy can help correct these hidden habits.
Swallowing is a fundamental habit that most of us take for granted. However, improper swallow patterns, often called “tongue thrust” can lead to a variety of dental and health issues. In myofunctional therapy, addressing these issues is key to achieving better overall health. In this week’s blog we will explore the importance of proper swallow techniques and the issues that an improper swallow technique can create. As well as how myofunctional therapy can help correct these hidden habits.
A proper swallow involves the correct positioning and movement of the tongue and other oral structures and is free from compensations.
During a proper swallow:
The tongue should rest against the roof of the mouth
The lips should be closed, and the teeth should come together slightly
The muscle of the face should remain relaxed
In an improper swallow, such as a tongue thrust, occurs when the tongue pushes against the teeth or comes forward between the teeth during swallowing. It does not always have to push forwards only. It can spill out of the sides of the teeth as well. This can lead to dental issues, speech concerns, facial developmental issues, digestive problems, impact breathing patterns, pain in the head neck region and affect sleep.
Why is a proper swallow important?
Dental Health: Improper swallow patterns can cause the misalignment of teeth, leading to malocclusion and other orthodontic problems. This increases the likelihood of needing braces, expansion, or other orthodontic interventions.
Facial Development: Over time, tongue thrusts can affect the development and alignment of the jaw and facial structures. This can lead to temporomandibular joint (TMJ) disorders, which may cause pain and discomfort.
Speech: Proper tongue posture and swallowing can influence speech and clarity.
Digestive Concerns: When we have our mouth open during the eating process we take in more air. This can lead to more acid reflux, bloating, gas, ect. When our tongue is not up in the palate during swallowing and instead pushing forwards, this will likely lead to more digestive issues such as GERD.
Breathing: A proper swallow pattern encourages nasal breathing, which is crucial for optimal oxygen intake and overall respiratory health.
Sleep: We are going to take a bigger dive into this one. Tongue thrusts can significantly impact sleep in several ways: Airway Obstruction: An improper swallow can lead to an improper resting posture of the tongue. When the tongue is in the improper position during sleep this can obstruct the airway. An obstruction in the airway can then lead to things such as: breathing difficulties, obstructive sleep apnea, snoring, and disturbances in quality and quantity of sleep. Mouth Breathing: Tongue thrusts often accompany mouth breathing habits. As discussed in previous blogs, nasal breathing is far better for our health than mouth breathing.
So now that we know how much our swallow can impact our health, let’s discuss how/why improper swallow patterns form. There are many reasons why and how these irregularities can form and we will not go into depth on all of them here.
Some of the reasons a tongue thrust can form:
prolonged pacifier, bottle, or sippy cup usage
structural issues like a high narrow palate
oral restrictions (tongue ties)
history of thumb sucking
chronic mouth breathing that could be related to enlarged tonsils, allergies
lack of awareness
neurological conditions
How Myofunctional Therapy Helps:
Myofunctional therapy focuses on retraining the muscles of the mouth and face to improve functions like swallowing:
Here’s how it can help:
Assessment: A thorough evaluation by a myofunctional therapist can identify improper swallow patterns and other related issues.
Exercises: Tailored exercise can strengthen the muscles involved in swallowing and encourage proper tongue posture.
Habit Correction: Myofunctional therapy provides guidance on eliminating habits like thumb sucking or mouth breathing that may contribute to improper swallow.
In conclusion, correcting an improper swallow pattern may seem like a small detail, but it can have a big impact on your overall health and well-being. Myofunctional therapy offers a comprehensive approach to identifying and correcting these hidden habits, paving the way for better dental health, improved breathing, more effective sleep, less GI symptoms, reduction in mouth breathing and a healthier you!
Eat With Your Mouth Closed & Chew Your Food: How the Way We Eat Can Impact Our Health & Development
How chewing with your mouth open, eating softer foods and improper eating habits can impact our jaw and facial development leading to more oral and heath issues.
Have you ever thought about the way you eat? Maybe as a kid you were told to chew with your mouth closed or to not talk with food in your mouth. Although these are ingrained in most of our minds as what is expected in society, we might not have realized there is a functional reason we should be performing these habits while eating. Let’s dive into eating and chewing, and how if done improperly, these tasks can impact our oral and overall health.
When we eat and chew we should ideally be able to do these tasks with our mouth closed. If we have to eat and chew with an open mouth it could be related to inadequate nasal breathing. There could be dysfunction in the mouth within the muscles. Open mouth chewing could be related to the anatomy of our structures. Additionally, there could be tension under the tongue impacting the way we chew and eat. A myofunctional therapist can help get to the root of the cause and why there are flaws in the way someone is eating and chewing.
Before we dive into it I want to start with a definition of epigenetics. “Epigenetics is a field of dentistry that studies how environmental factors affect the genes that control jaw development. Epigenetics adds a layer of complexity to genetics, which provides the blueprint for facial structure, by showing how external factors like lifestyle, habits, and environmental stimuli can influence how genes are expressed. For example, the way a person breathes, swallows, and chews can impact the growth and development of their jaw and facial bones.”
So why does this matter? If we chew with our mouth open we tend to take in more air leading to more GI symptoms such as: gas, bloating, burping, hiccups, acid reflux, and more. When we limit hard to chew foods, this can impact the way our face and jaws are formed. Our jaws, like the rest of our body, need to be continuously worked. When we feed our children soft foods we don’t work the muscles and jaw as much as they need to be. This reduction in chewing tough foods starts to create narrower jaws in people. Scientists have studied skulls from the stone age to help understand this concept. They discovered the skulls of our ancestors had large, broad jaws and were able to accommodate all 32 teeth including the wisdom teeth. As the scientists compared the jaws to those of today, they noted a significant decrease in size of the jaw. The majority of the jaws were not able to fit all the teeth. Many people in our modern society have to get their wisdom teeth removed due to lack of space. A large number of people are also recommended to have other permanent teeth removed due to lack of space. An entire blog will be written on this; however, when we remove permanent teeth due to lack of space we create a more narrow jaw and subsequently smaller airways.
What would be the reason that scientists have found this analysis in our prehistoric jaws and jaws of today? There are several reasons, but we are going to specifically speak about chewing and eating tough vs. soft foods. In the days of our ancestors they did not have the capability to soften and pulverize their food like today. Much of what they ate required vigorous chewing. Today we now have the introduction of many ways to soften, smash and create foods that we do not have to chew as much. As early as 4 months we are told to begin giving our babies purees. Don’t get me wrong, I am all for a mix of purees and solid foods. It’s all about a balance. However, when we begin to eat many more foods that we do not have to chew, we start to really impact the way our facial structures are formed and they can be negatively affected. Additionally, we now have many more tools that have made eating and drinking easier, although they can impact our development. This would include tools like sippy cups, bottles and more.
So what can we do to help? First, if you suspect there is a dysfunction with the way you or someone is eating, begin by scheduling an evaluation with a myofunctional therapist. They can help you get to the root of the cause of dysfunctional chewing and eating. Next, encourage habits that aid in muscle strength and oral development. Breastfeeding has one of the best effects on oral motor development. Breastfeeding may not work or be possible for everyone, so bottle feeding using specific bottles and feeding techniques like “paced feeding” can assist in oral motor development. Once our little ones are ready to introduce solids, following baby led weaning protocols can help progress oral molar function. And when our little ones are ready for tougher foods, encouraging them to eat harder to chew food. Foods such as jerky and fruit leathers are excellent for strengthening our jaws. Additionally, if it is functionally possible to chew with your mouth closed while breathing through your nose, do so. Finally, SLOW DOWN your eating habits. We should be chewing our food at least 20 times after eating before we are attempting to swallow. Lastly, swallow correctly. This is another topic to cover completely, so stay tuned. A proper swallow pattern is critical to our oral and overall health. Hint, if you or someone you know has been told you have a reverse swallow pattern or a tongue thrust, that is not a proper swallow pattern and will lead to many issues. To summarize, begin by introducing proper and healthy functions as early as bottle or breastfeeding. Next, begin to feed your little one solids by following the baby led weaning protocol. Following that, encourage your child to eat tougher to chew foods. Lastly, aim to have proper eating habits such as slow eating while keeping your mouth closed. These practices will assist in less health ailments and reduce improper jaw and facial development.
Oral Habits When We Are Young Can Lead to a Lifetime of Health Issues
Toxic oral habits can significantly impact oral development, particularly in children. These are habits such as: thumb sucking, prolonged pacifier/bottle use, and nail biting. They can lead to a lifetime of health issues such as: poor sleep, mouth breathing, malocclusion, snoring, sleep apnea, digestive issues, congestion, the need for braces or expansion, behavior issues, improper jaw development, grinding/clenching, head and neck pain, and more.
Let’s talk about “oral toxic habits,” AKA harmful oral habits that can significantly impact the oral development, particularly in children. These are habits such as: thumb sucking, prolonged pacifier/bottle use, and nail biting. Not only can these habits influence our teeth, they can also affect someone’s overall health. Yes, pacifiers serve a purpose in the early months to assist with sleep and are shown to prevent SIDS; however, after 4 months they can begin to cause more damage than good. The best way to use a pacifier is to only use it to assist with sleep and not during the awake periods. By 4 months swap the pacifier out with teethers or tools such as the MyoMunchee.
Oral habits when we are young can lead to a lifetime of health issues such as: poor sleep, mouth breathing, malocclusion, snoring, sleep apnea, digestive issues, congestion, the need for braces or expansion, behavior issues, improper jaw development, grinding and clenching, head and neck pain, and more.
Why are these aids and habits so harmful to our health? As our jaws and teeth are developing and erupting we are designed to have the tongue in the roof of our mouth to help create a wide upper palate and put pressure on the teeth as they erupt. The pressure of the tongue helps to prevent the teeth from shifting inwards and crowding (which is what they naturally want to do). When we have a foreign object in the mouth for prolonged periods such as a pacifier, bottle, or fingers we are preventing the tongue from being up in the roof of the mouth. These habits can all have a significant impact on our occlusion (how our teeth come together). We often see open bites, very narrow upper palates and malocclusion (teeth overlapping, delayed eruption, recommended to get teeth pulled due to space) in individuals who have/had an oral habit. This usually leads to someone needing braces/ortho, expanders and appliances in the future to restore the damage that has been done. Unfortunately, the damage will follow us into adulthood unless we also change the function.
Pacifiers should not be a replacement for our tongue.
Additionally, when we have an object in the mouth resting up on our palate other than the tongue, our tongue is hanging low. When our tongue is hanging low and in the improper position this will impact our ability to breathe properly. This can create a habit of mouth breathing. Consequently, this can lead to congestion, sleep issues, postural issues, increased sickness and more. When our tongue is hanging low, instead of up in the roof of the mouth, where it is intended, this then drags the rest of our face back and downwards. We often see small, set back chins in individuals who have a low tongue resting posture. We also typically see narrow airways that can lead to breathing disorders.
Thumb sucking can be a sign of a tongue tie.
In some situations people compensate with oral habits because their tongue is physically unable to be on the roof of their mouth. We often see thumb or finger sucking arise in individuals who have a tongue tie. Sometimes someone might begin thumb sucking as a calming tactic related to stressors in life. In circumstances of those who have a tongue tie, this is because their tongue is being pulled or restricted to the floor of the mouth and the tongue is unable to be up in the palate where it belongs. Correct tongue posture is critical for stimulation of the vagus nerve. The Vagus nerve is responsible for rest/digestion, calming the body after stress and to exit fight or flight, respiratory response, heart rate and more. When we are not getting enough of that stimulation from our tongue, the body finds a way to receive that stimulation another way. People may begin to thumb suck to get the stimulation they are missing out on. Instead of using our fingers to get the stimulation, myofunctional therapy can help people begin to teach their tongue to be in the proper position and stimulate the vagus nerve.
Ideally we should wean from bottles to an open cup between 6 months to a year.
So how can we help or prevent these oral toxic habits? First, it all starts with proper function during infancy. By working with myself or another provider trained on oral dysfunction, we can assess to see if there is tension present, low tone in the oral/facial muscles or improper habits. We can help with breast or bottle feeding to ensure that they are both creating the best oral function. We can help with weaning the pacifier and offering better, more beneficial tools for oral development. If low tongue posture is present, we can work with individuals to create the proper tongue resting posture. If braces are needed we can work alongside an orthodontist to ensure that once we have shifted the teeth and the bone, we also retrain the muscles so the teeth won’t shift back after completion of ortho. Myofunctional therapy works a lot like physical therapy. If we need an ACL surgery, we pair it with physical therapy to rehab the knee after surgery. Same with our mouth. If we need a tongue tie procedure, braces, or an oral appliance we also need to pair those with myofunctional therapy to retrain the muscles of our mouth and create proper habits and functions.
We Are Designed to be Nasal Breathers, NOT Mouth Breathers
We are designed to breath through our nose, not our mouth. Learn the benefits of nasal breathing vs. mouth breathing and how myofunctional therapy can assist in this goal.
Yes, we can breath through our mouth, but are we supposed to? NO. The health benefits of breathing through our nose far outweigh the negative implications that breathing through our mouth has. There are several reasons that someone might begin to breath through their mouth, so we often must address that first in therapy before can achieve our goal of nasal breathing. Someone might have a blockage in the nasal cavity related to nasal polys, a deviated septum, or enlarged turbinates. An individual could have enlarged tonsils or adenoids. The reason could be related to prolonged pacifier and/or bottle use. Sometimes there is a restricted lingual frenum or “tongue tie” present. There might be a birth abnormality. Finally, chronic congestion might be present related to allergies, colds or sinusitis.
Let’s discuss why mouth breathing is detrimental to our health vs. nasal breathing. Our mouth is predetermined to be used for eating or speaking, not breathing. There are situations we might need to breath through our mouth, but only as a backup, not as the primary location. When we breath through our mouth our tonsils and gum tissues act as the filter for the cold, polluted air. This creates these tissues to often become enlarged, red and sometimes infected. When we breath through our mouth our body enters a state of fight or flight that affects our ability to rest and digest. Additionally, breathing through our mouth causes chronic congestion. The body assumes that C02 is being lost too quickly, so it signals the goblet cells to produce mucus in the nose to slow down the breathing. This creates a cycle of chronic congestion.
We often see more grinding and clenching in those who primarily breath though their mouth. We also see more issues with the TMJ. Those who mouth breath will typically have a forward head posture and often have improper jaw development. It is common to see crowding of the teeth and malocclusion in those who mouth breath. There is an increased risk for ear infections in someone who mainly breaths through their mouth. Furthermore, there is no release of nitric oxide when breathing through the mouth. Nitric oxide has anti inflammatory and anti bacterial benefits. Those who continuously breath through their mouth are generally going to get sick more often. Also, breathing through our mouth can alter sleep and increase our risk for obstructive sleep apnea.
Conversely, nasal breathing is far superior for our health. The nose warms and humidifies the air, which increases the efficiency of the lungs. Nasal breathing releases nitric oxide to help the body have anti bacterial and anti inflammatory benefits. The nose filters out the allergens and bacteria first, so they are less likely to enter the body. Additionally, nasal breathing helps with relaxation and our rest and digest systems. Plus nasal breathing helps with sleep. Less night wakings, more restorative sleep and less snoring!
Once we address why someone is chronically mouth breathing we can begin to work on nasal breathing in myofunctional therapy. By targeting the function and increasing the tone of the muscles of the jaw, lips, tongue, soft palate and larynx we can help to ensure that nasal breathing is the primary form of breathing in individuals. By breathing through our nose we can feel better, sleep more and get sick less!
Obstructive Sleep Apnea
Myofunctional therapy to treat obstructive sleep apnea
There is a misconception that sleep apnea only impacts older, overweight men. We also know that obstructive sleep apnea is grossly under diagnosed and treated. Obstructive sleep apnea, or OSA, can affect any age, any size and any gender. Babies can even have sleep disordered breathing. Children will show signs of sleep disordered breathing as: having night terrors, behavioral issues, prolonged bed wetting, snoring, grinding/clenching at night, have chronic congestion or other signs. Adults will often show signs in the mouth. They might have bad breath, their tongue hangs low, or they get frequent cavities not related to sugar consumption. These individuals might have a smaller chin that is set back. They might mouth breath, snore, grind/clench or have pain in the head and neck. These folks are often very tired during the day. Those who have a level of sleep apnea will experience microarousals, or brief awakenings. This might look like someone waking up to pee, rolling around in their sleep, gasping for air, or grinding/clenching. The severity of sleep apnea is determined by how often breathing is interrupted during sleep, and is measured by the apnea-hypopnea index. These sleep apnea events occur 5-15 times in an hour in mild OSA, 15-30 times in moderate and more than 30 times in severe OSA. This means someone who has severe OSA is “waking up” more than 30 times in an hour! There is a reason this person is waking up feeling like they got little to no sleep, it is because they didn’t. Their body was in a constant state of fight or flight. They hardly get any good, restorative, deep sleep. Being tired is one thing, but OSA can be a risk factor for many other health concerns such as: high blood pressure, type II diabetes, liver issues, among others.
So, what can you do about it? One option is a CPAP machine. These can be bulky, annoying to transport/travel with and compliance is generally low with these machines. There are surgeries that can help with some of the underlying causes. There are appliances that you can wear at night that help position the tongue in the correct resting posture and finally there is myofunctional therapy. This is where we can help. As Myofunctional Therapists, we assess the function of the oral/facial muscles and we can uncover where there is dysfunction. We can build strength in the muscles of the mouth to help get the tongue resting in the proper position. Finally, we build proper habits to help reduce these microarousals. We can help you to breath and sleep better and in return FEEL BETTER!
Myofunctional Therapy to Treat Obstructive Sleep Apnea